Posted by: Batchelet Eye in Cataract Surgery,Cataracts

If the world looks a little hazier than it used to — like you’re peering through a foggy windshield that no amount of wiping will fix — you’re not imagining things. And you’re certainly not alone. Cataracts affect roughly half of all Americans by age 80, and if you’ve been told you have one, the natural next question is: now what?
The good news is that cataract surgery is one of the safest and most successful procedures in all of medicine. Dr. Andy Batchelet has personally performed over 25,000 of these surgeries, and the vast majority of patients walk away seeing more clearly — often by the very next morning.
This guide walks you through everything you need to know, from what’s actually happening inside your eye to what recovery looks like — so you can make a confident, informed decision about your vision.
What Is a Cataract?
Your eye has a natural lens that sits behind the pupil, much like the lens inside a camera. Its job is to focus light onto the retina so you can see clearly. A cataract forms when the proteins in that lens begin to break down and clump together, creating a cloudy patch that blocks and scatters light.
Think of it this way: imagine looking through a clean window versus a window that’s been slowly fogging up from the inside. That’s essentially what’s happening — except the “window” is inside your eye, and no amount of cleaning from the outside will fix it.
At Batchelet Eye, many patients are surprised to learn how gradually this happens.
“A lot of people tell us they didn’t realize how much their vision had declined until we showed them,” is something we hear almost daily in clinic.
Cataracts develop gradually, often over years, and most people don’t even notice the early stages. But over time, the cloudiness grows, and so does the frustration.
What Causes Cataracts?
Aging is the primary culprit. After about age 40, the proteins in your lens naturally begin to break down. But several other factors can speed up the process:
- Diabetes — elevated blood sugar can cause lens changes earlier in life
- Smoking — significantly increases cataract risk
- Prolonged sun exposure — UV radiation damages the lens over time
- Certain medications — long-term steroid use is a well-known contributor
- Eye injuries or previous eye surgery
- Family history — genetics play a role for some patients
Even if none of these apply to you, cataracts can still develop simply because of the passage of time. It’s one of the most common age-related changes in the human body.
How Do Cataracts Affect Your Daily Life?
Cataracts rarely announce themselves with a single dramatic moment. Instead, the changes creep in gradually — which is why many patients tell us, “I didn’t realize how bad it had gotten until after surgery.”
Common Symptoms to Watch For
- Blurry or cloudy vision — as if looking through a frosted or smudged window
- Faded or yellowed colors — whites may appear cream-colored; reds and blues lose their vibrancy
- Increased glare sensitivity — bright sunlight or oncoming headlights become uncomfortable or even blinding
- Halos around lights — streetlights and headlights seem to sprout rings or starbursts, especially at night
- Difficulty reading — fine print requires brighter light or a magnifying glass
- Frequent prescription changes — your glasses never seem quite right anymore
- Double vision in one eye — an unsettling “ghosting” effect that can come and go
What Cataract Vision Actually Feels Like

Patients describe it in ways that are immediately relatable:
- “Like wearing dirty sunglasses you can’t take off” — everything is dimmer and slightly out of focus
- “The world looks washed out” — colors that used to pop now feel muted and flat
- “Driving at night became terrifying” — headlights explode into blinding starbursts with rainbow-like rings
One of the most striking things patients tell us after surgery is how they didn’t fully appreciate what they were missing. “I had no idea my white kitchen walls had turned yellow” is something Dr. Batchelet hears regularly.
When Is the Right Time for Surgery?
This is one of the most common questions patients ask — and the answer may surprise you.
There’s no rule that says you need to wait until your cataract is “ripe” or “mature.” That’s an outdated idea from decades ago when surgical techniques were less refined. Today, the right time for surgery is when your vision starts interfering with the things that matter to you.
Ask yourself:
- Is reading becoming a struggle, even with good lighting?
- Do you feel unsafe driving, especially at night?
- Are hobbies like gardening, sewing, or woodworking harder to enjoy?
- Do you avoid social situations because you can’t see faces clearly?
If you answered yes to any of these, it may be time to have a conversation with your ophthalmologist.
Waiting too long doesn’t usually harm the eye itself, but it does mean living with unnecessarily poor vision — and in some cases, very advanced cataracts can make the surgery slightly more complex. There’s no prize for waiting, and there’s a lot to gain from acting when you’re ready.
How Cataract Surgery Works
Here’s where many patients breathe a sigh of relief: cataract surgery is not the intimidating ordeal people often imagine. It’s a quick, outpatient procedure that typically takes just 10 to 20 minutes per eye.
The Procedure, Step by Step
- Your eye is numbed with anesthetic drops — no needles near your eye in most cases
- A tiny incision is made in the cornea, usually just a few millimeters wide
- The cloudy lens is gently broken up using ultrasound energy (a technique called phacoemulsification) and removed
- A clear artificial lens (IOL) is inserted through the same small opening, where it unfolds and settles into place
- The incision seals on its own — no stitches needed in the vast majority of cases
You’ll be awake during the procedure, but a mild sedative helps you stay relaxed and comfortable. Most patients say they see some light and movement but feel no pain — just a slight sensation of pressure.
What About Dropless Cataract Surgery?
Traditionally, patients go home with several bottles of eye drops and a complex schedule to follow for weeks after surgery. For older patients especially, this can be confusing and frustrating.
At Batchelet Eye, Dr. Batchelet frequently uses an advanced dropless technique. During the procedure, medication is placed directly inside the eye, which means:
- No complicated drop schedule
- Less risk of missing doses
- A simpler, more comfortable recovery
For many of our patients — especially those who live alone or have difficulty with drops — this has been a meaningful improvement in their overall experience.
Understanding Your Lens Options
Choosing your lens is one of the most important parts of the process — because it shapes how you’ll see after surgery. Think of it like choosing a new camera lens: each type has different strengths.
At Batchelet Eye, this is never rushed. We take time to understand your lifestyle, your goals, and what matters most to you.
Monofocal Lenses
The standard option, covered by Medicare and most insurance plans. A monofocal lens focuses at one distance — usually far away. Depending on the shape of your eye, you may require glasses at all times after surgery even if you didn’t require them in certain situations before. Even with the ideal eye shape, you will need reading glasses for the computer, books, menu, and your phone.
For many patients, this is a perfectly good choice especially if you are comfortable wearing glasses.
Toric Lenses
If you have astigmatism (an irregular curve in your cornea that blurs vision at all distances), a toric lens corrects that during surgery. Many patients who choose a toric IOL are thrilled to find they no longer need distance glasses for the first time in years. Reading glasses are still required for all near tasks with this lens. This lens involves an additional out-of-pocket cost.
Multifocal and Extended Depth of Focus (EDOF) Lenses
These premium lenses are designed to give you clear vision at multiple distances — far, intermediate, and near — reducing your dependence on glasses overall. They’re a popular choice for active patients who want maximum freedom from eyewear.
These lenses do involve additional out-of-pocket cost, and they’re not ideal for every eye. Dr. Batchelet takes time during your consultation to discuss which lens matches your eyes, your lifestyle, and your expectations.
The Light Adjustable Lens (LAL)
This is one of the most exciting advances in cataract surgery today. Unlike traditional IOLs, the Light Adjustable Lens can be fine-tuned after surgery using painless light treatments in the office.
Why does that matter? Because even with the best pre-surgical measurements, every eye heals a little differently. The LAL lets your surgeon optimize your prescription after the lens is already in place — giving you a level of precision that simply wasn’t possible before. A large percent of patients who receive this lens see better than 20/20.
Dr. Batchelet is one of only four surgeons in Western Pennsylvania offering the Light Adjustable Lens, making this technology accessible to patients who would otherwise have to travel to a major city.
What to Expect During Recovery
Recovery from cataract surgery is faster than most patients expect. Here’s a realistic timeline:
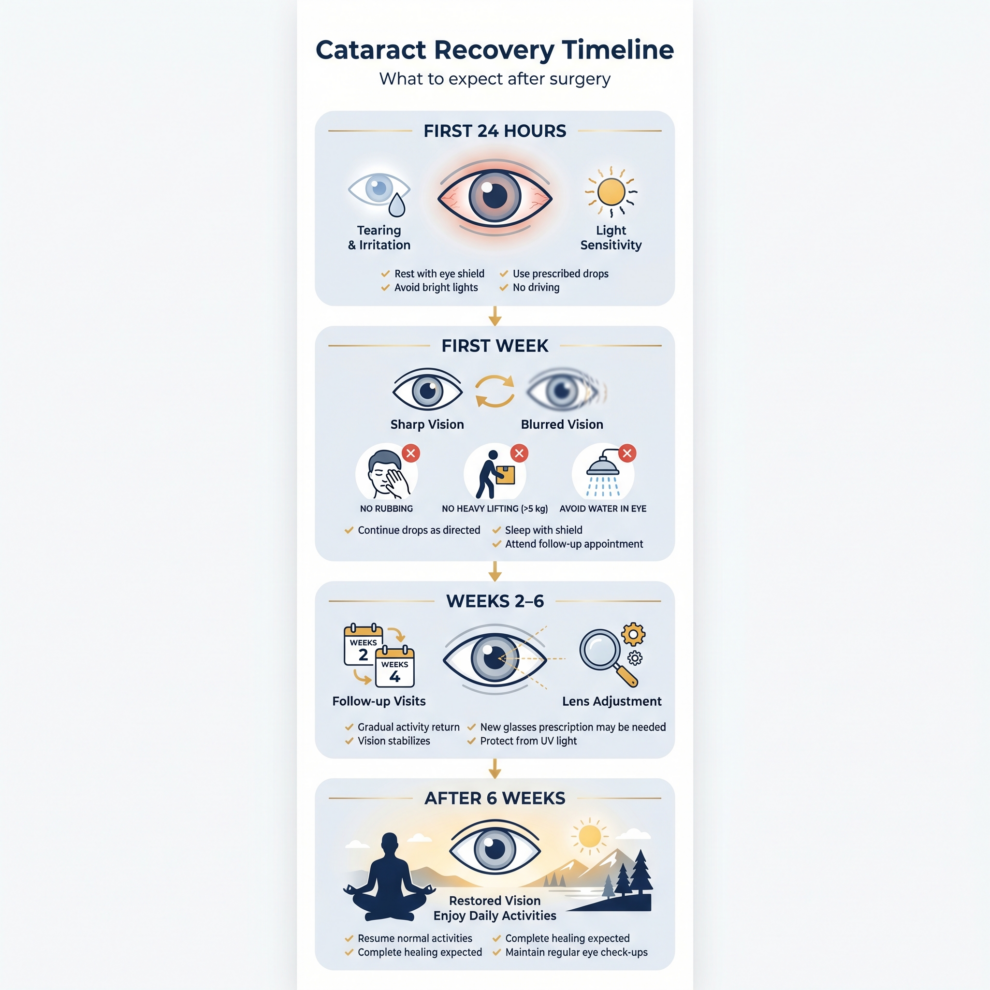
The first 24 hours: Your eye may feel scratchy, watery, or slightly sensitive to light. This is normal. Many patients notice significantly clearer vision by the next morning — sometimes dramatically so.
The first week: Vision continues to improve daily. Some patients experience mild fluctuations — slightly clearer one day, a touch blurry the next — as the eye settles. Avoid rubbing your eye, heavy lifting, and getting water directly in your eye.
Weeks two through six: The eye completes its healing. You’ll have follow-up visits so Dr. Batchelet or your referring doctor can monitor your progress and, if you chose the Light Adjustable Lens, begin the fine-tuning adjustments during this window.
After six weeks: Most patients are fully healed and enjoying their best vision. If both eyes need surgery, the second eye is typically done one to two weeks after the first.
Recovery Tips
- Arrange a ride home from surgery — you won’t be able to drive that day
- Wear the protective eye shield at night for the first week
- Use prescribed drops as directed (unless you’ve had the dropless procedure)
- Avoid swimming, dusty environments, and strenuous exercise for a few weeks
- Don’t hesitate to call the office if anything feels off — that’s what we’re here for
Common Myths About Cataract Surgery
There’s a lot of outdated information floating around. Let’s set the record straight.
“Cataracts can grow back after surgery.”
They cannot. Once your natural lens is removed, it’s gone for good. The artificial lens that replaces it does not develop cataracts. In some cases, the thin membrane behind the lens can become slightly hazy months or years later — but this is easily corrected with a quick, painless laser treatment in the office.
“The surgery is extremely painful.”
It isn’t. The eye is thoroughly numbed, and patients receive a mild sedative. Most people feel only slight pressure and describe the experience as far easier than they expected.
“You need to wait until you’re nearly blind.”
This is one of the most persistent — and most harmful — myths. Modern cataract surgery can be performed safely at any stage. Waiting only means living with poor vision longer than necessary.
“It’s major surgery with serious risks.”
Cataract surgery is an outpatient procedure, not major surgery. Serious complications occur in fewer than 1% of cases. It’s one of the most frequently performed and safest operations in modern medicine.
“I won’t need glasses at all after surgery.”
This depends on the lens you choose. Standard monofocal lenses provide excellent distance vision but usually require reading glasses. Premium lenses reduce glasses dependence significantly, but even with the best technology, some patients prefer glasses for certain tasks. Honest expectations lead to the happiest outcomes.
Frequently Asked Questions
No. Your eye is numbed with anesthetic drops, and you’ll receive a mild sedative to keep you relaxed. Most patients feel only light pressure during the procedure. Afterward, the eye may feel slightly scratchy or tired for a day, but significant pain is uncommon.
The procedure itself typically takes about 10 to 20 minutes per eye. You’ll spend additional time at the surgery center for preparation and a brief recovery period before heading home.
You should not drive on the day of surgery. Most patients can resume driving within a few days, once vision has cleared and your doctor confirms it’s safe — usually at your first follow-up appointment.
Having another eye condition does not automatically disqualify you from cataract surgery. In many cases, removing the cataract actually helps your doctor better monitor and manage other conditions. Each situation is evaluated individually.
No. Age alone is not a barrier. Dr. Batchelet regularly performs cataract surgery on patients in their 70s, 80s, and even 90s. As long as you’re healthy enough for a minor outpatient procedure, surgery is an option.
The cataract will continue to worsen over time. You can manage symptoms temporarily with stronger glasses, brighter lighting, and magnifiers, but these are stopgap measures — surgery is the only way to restore the vision a cataract takes away.
If both eyes have cataracts, then yes — each eye is treated separately. Typically, the second eye is scheduled one to two weeks after the first, giving the first eye time to heal.
Preparation is minimal. You’ll have a pre-operative visit for eye measurements, and you’ll receive simple instructions about medications and eating beforehand. The most important things: arrange a ride home and plan to rest on surgery day.
Take the Next Step Toward Clearer Vision
If cataracts are making your world look a little dimmer than it should, you don’t have to just live with it. A conversation is the first step — no pressure, no commitment, just a chance to understand your options and ask every question on your mind.
Dr. Batchelet and the team at Batchelet Eye are here to give you the information you need to make the best decision for your eyes and your life. With three convenient locations across Western Pennsylvania — in Grove City, New Castle, and St. Marys — expert care is closer than you think.
Schedule a cataract consultation today
and find out what clearer, brighter vision could look like for you.
